 
Disruption of growth and bone deformity (especially Salter-Harris types III–V).Salter-Harris type V: Treatment depends on age of injury at diagnosis.Surgical intervention includes open reduction and internal fixation (osteosynthesis) using wires or traction screws, followed by immobilization with a cast.Open reduction is required to realign the joint surface because both these types affect the joint.In case of severe dislocation or concomitant injury: surgical intervention (as performed in Salter-Harris types III and IV ).Closed reduction if displaced and immobilization in a cast with reevaluation after 7–10 days.MRI: may be helpful if radiographic findings inconclusive.X-ray (AP and lateral views) : Physeal widening may be the only finding. 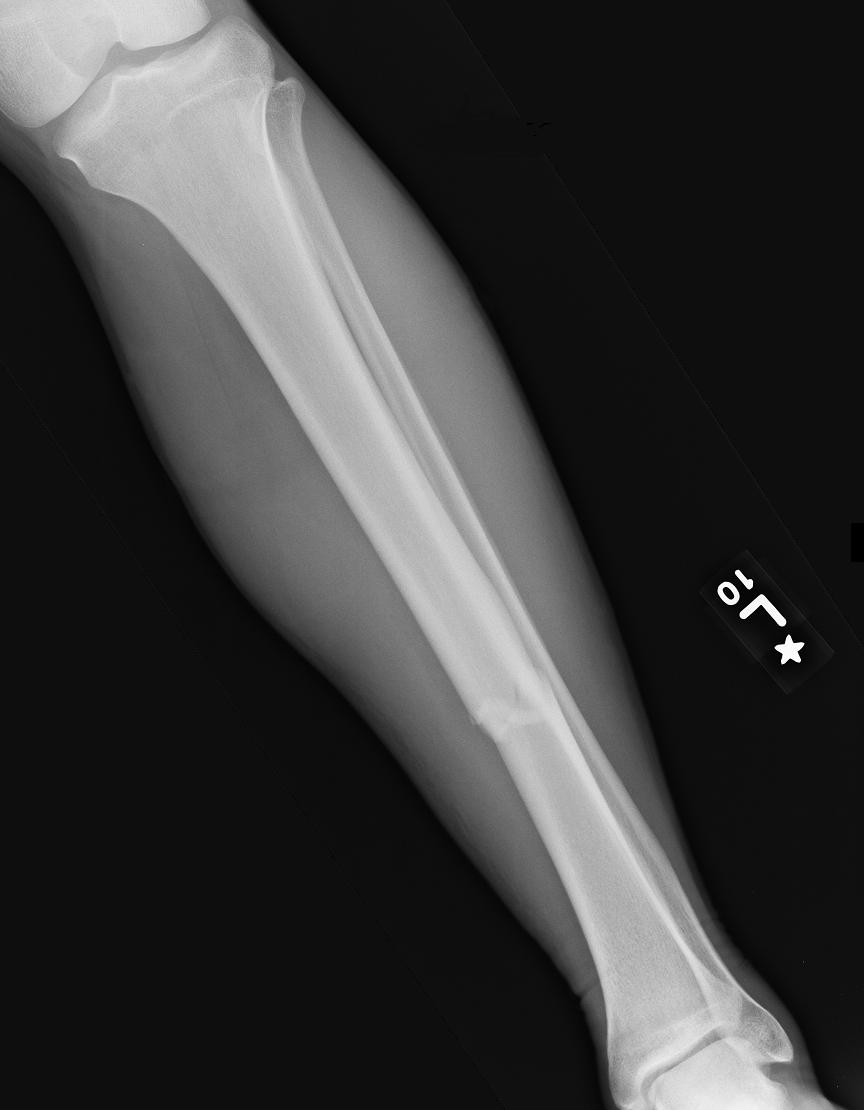
SALTER: S – straight across the joint ( type I) A – above the joint ( type II) L – lower ( type III) TE – through everything ( type IV) R – ruined or rammed ( type V) Type V: fractures characterized by impaction and disruption of the physis occur due to a crush or compression injury.Type IV: fractures through the metaphysis, physis, and epiphysis, that enter the joint.Type III: transverse fractures of the physis and epiphysis may extend to the joint and affect the articular surface.Type II: transverse fractures of the metaphysis and physis, which often involve separation of a triangular section of the metaphysis most common type of Salter-Harris fracture.Type I: transverse fractures of the physis, separating the epiphysis from the metaphysis.Mild clinical symptoms may lead to misdiagnosis. Inability to bear weight on the injured side.Focal tenderness to palpation around the physis.History of trauma (e.g., fall or collision).Most common sites: distal radius and the distal humerus.Peak incidence : : most frequently occur during growth spurts at the beginning of puberty ( 11–12 years for girls and 13–14 years for boys ).Definition: physeal or growth plate fracture.Minor angulations in pediatric fractures do not require manual reduction because they are often compensated during remodeling and growth. In greenstick fractures, the bone bends and breaks like a green (young) stick. > 10 years: lateral view: 5–15° AP view: 0°.Diaphysis of the ulna (most common) or fibula.No disruption of the cortex or periosteum.Greater than acceptable angulation: closed reduction followed by immobilization with a cast. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
